Pharmacy Training and Development: Building a High-Quality Primary Care Workforce
4th February 2026
Ongoing pharmacy training is critical in primary care as clinical complexity increases and pharmacy roles continue to expand across practices and PCNs. Without structured, role-specific development, teams can struggle with confidence, consistency, and prescribing safety. Targeted training ensures pharmacy teams are equipped to deliver safe, effective care while supporting long-term workforce quality and retention.
We consistently see that structured, role-specific training is what enables pharmacy teams to deliver safely and confidently in primary care. When development is aligned to real service demand, it strengthens patient safety, team resilience, and long-term workforce quality.
Adeem Azhar, Co-Founder and Chief Executive Officer – Core Prescribing Solutions
- What Do We Mean by Pharmacy Training in Primary Care?
- Why Training and Development Matter for Workforce Quality
- Core Areas of Clinical Skills Development for Pharmacy Teams
- Identifying Capability Gaps in Pharmacy Teams
- How Targeted Training Improves Capability in Practice
- Training as a Retention and Workforce Sustainability Tool
Key takeaways
- Targeted pharmacy training improves clinical confidence and consistency across practices and PCNs.
- Ongoing skills development supports safer prescribing and more efficient patient care.
- Structured training pathways improve retention by giving pharmacy teams clarity, confidence, and progression.
What Do We Mean by Pharmacy Training in Primary Care?
Pharmacy training in primary care refers to ongoing, role-specific development that goes beyond initial qualification. It includes building clinical, operational, and system skills needed to work effectively within GP practices and PCNs. The focus is on practical capability and confidence in day-to-day delivery, rather than theoretical learning or generic CPD activity.

Why Training and Development Matter for Workforce Quality
Primary care pharmacy roles continue to expand across practices and PCNs, increasing the need for structured training and supervision to support safe, consistent delivery. This reflects NHS England guidance on primary care pharmacy roles, which highlights the importance of developing clinical capability alongside workforce growth.
Training and development are central to patient safety and service consistency. When pharmacy teams are confident in their skills, they make safer clinical decisions and work more effectively within the wider MDT. Clear development pathways also improve retention by giving staff confidence, progression, and clarity in their role, strengthening service resilience and long-term workforce quality.
Core Areas of Clinical Skills Development for Pharmacy Teams
Effective pharmacy services in primary care rely on strong clinical skills across medicines optimisation, prescribing safety, and long-term condition management. Ongoing development supports safer decision-making and appropriate prescribing, in line with NICE guidance on medicines optimisation.
- Medicines optimisation and prescribing safety to support safe, effective, and appropriate use of medicines.
- Long-term condition management across areas such as cardiovascular disease, diabetes, and respiratory care.
- Prescribing safety and decision-making, including risk assessment and escalation.
- Consultation and communication skills to support shared decision-making and patient understanding.
- Use of clinical systems and data to manage workload, monitor outcomes, and support proactive care.
Identifying Capability Gaps in Clinical Pharmacy Teams
Identifying capability gaps early helps ensure pharmacy teams remain safe, effective, and aligned with service demand.
- Variation in confidence or competence across different clinical pharmacy roles and experience levels.
- Introduction of new roles or expansion of scope that requires additional skills and supervision.
- Feedback from incidents, audits, complaints, or clinical supervision highlighting development needs.
- Service pressures or changes in workload that expose gaps in skills or capacity.

How Targeted Training Improves Capability in Practice
| Step | What this involves in practice | Why it helps improve capability |
| Assess current capability | Review skills, confidence levels, and role expectations against current service demand. | Identifies where capability gaps exist and avoids unfocused training. |
| Prioritise training needs | Align training with PCN and system priorities, such as long-term conditions or medicines safety. | Ensures training effort supports real service pressures. |
| Deliver role-specific training | Provide structured training tailored to clinical pharmacists, pharmacy technicians, and support roles. | Builds relevant skills rather than generic knowledge. |
| Support learning | Reinforce training through supervision, mentoring, and peer review. | Helps staff apply learning safely and confidently in practice. |
| Embed into workflows | Integrate new skills into day-to-day systems, templates, and processes. | Sustains improvements and helps teams consistently improve capability over time. |

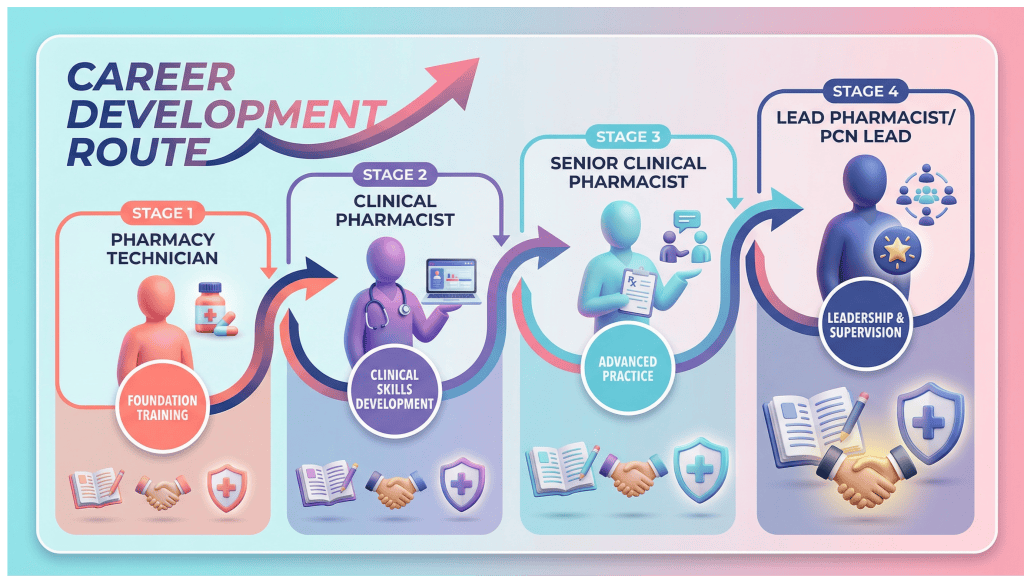
Training as a Retention and Workforce Sustainability Tool
Access to meaningful training and development improves staff engagement by helping pharmacy teams feel confident and valued in their roles. Clear development pathways reduce burnout linked to role uncertainty or scope creep, particularly in expanding primary care roles. Over time, structured training also supports progression within primary care, strengthening retention and contributing to a more sustainable workforce.
How Core Prescribing Solutions Can Help?
Core Prescribing Solutions supports primary care teams with pharmacy training programmes aligned to service needs. We provide clinical skills development support, carry out capability assessments and development planning, and link training directly to service delivery and quality improvement priorities.
Our approach focuses on building practical capability that supports safe, consistent, and sustainable care across practices and PCNs.


 01274 442076
01274 442076