The Hidden Cost of Staff Turnover in Primary Care
|
Getting your Trinity Audio player ready...
|
High attrition remains a persistent challenge across the NHS, but in primary care the impact is often more immediate and harder to absorb. Smaller teams and rising demand mean that when someone leaves, clinics are disrupted, workloads increase, and continuity of care begins to break down. Understanding the full cost of losing team members is essential for practices and PCNs looking to maintain stability and plan their workforce effectively.
Key Takeaways
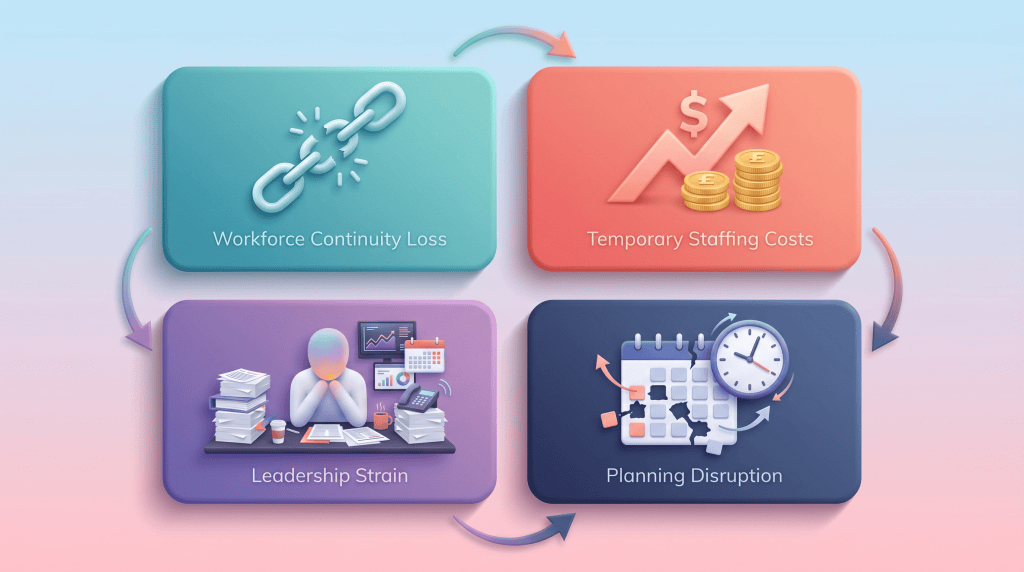
- Workforce continuity: Frequent departures disrupt patient relationships and care delivery, not just recruitment pipelines.
- Temporary staffing costs: High turnover increases reliance on locum and agency cover, raising costs and reducing consistency.
- Leadership strain: Management time is diverted from service improvement to constant backfilling.
- Planning disruption: Workforce planning becomes unreliable when teams are in constant flux.
What is staff turnover and why does it matter in primary care?
Staff turnover refers to the rate at which employees leave an organisation and need to be replaced. In primary care, even modest levels of turnover can have a disproportionate impact. Unlike larger hospital settings, GP practices and PCNs operate with lean teams and limited capacity to absorb gaps.
When roles such as Clinical Pharmacists in PCNs or Pharmacy Technicians are left unfilled, the effects are immediate: appointments are reduced, existing staff carry additional workload, and patient experience suffers. This churn is not just an operational metric – it is a key indicator of service stability.
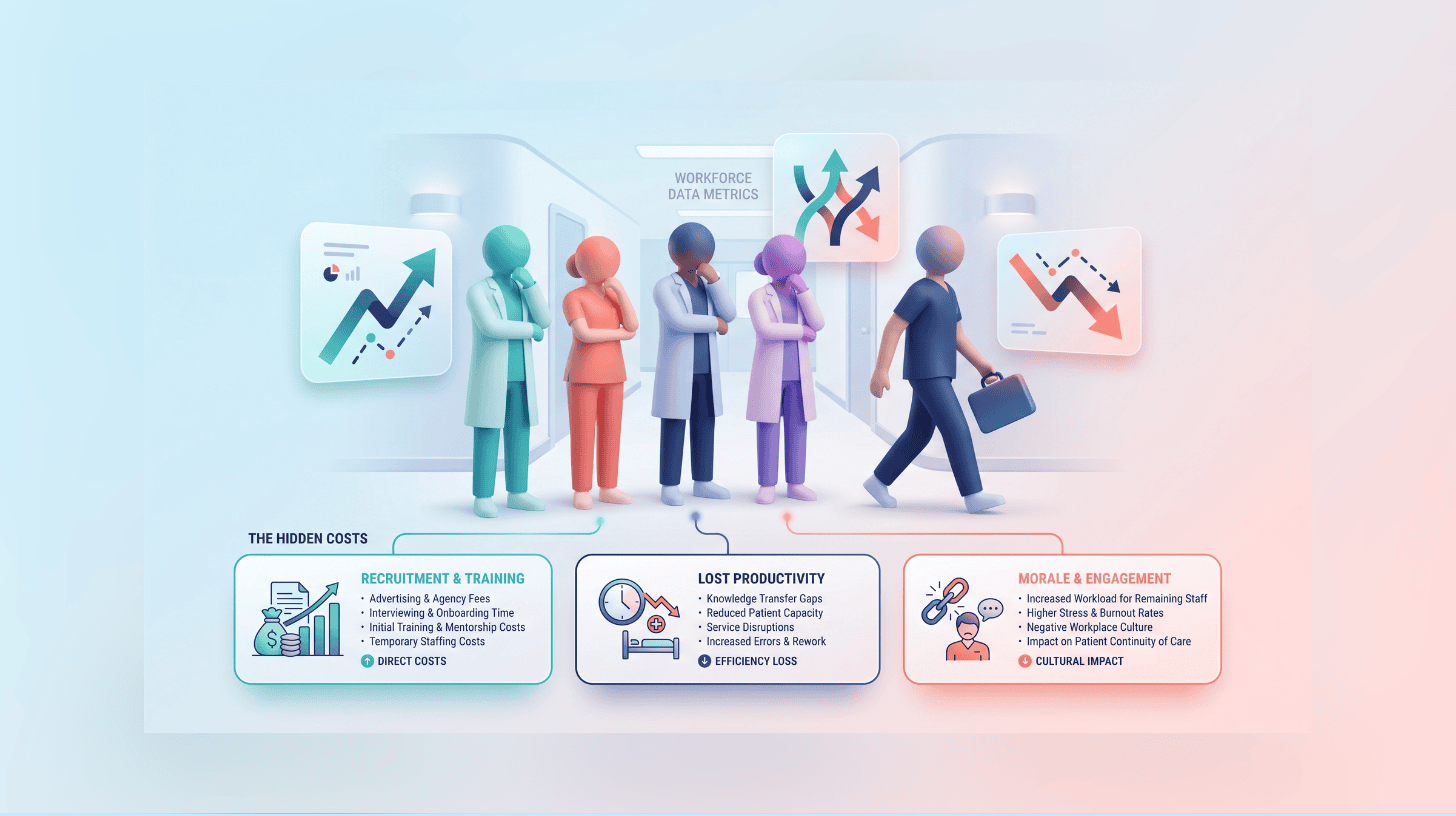
What are the hidden costs of staff turnover in primary care?
Loss of workforce continuity
When staff leave, patient relationships are disrupted, handovers become inconsistent, and local knowledge is lost. Over time, this erodes team confidence and weakens continuity of care – one of the most significant but least measured costs of high turnover.
Increased reliance on temporary staffing

A revolving door of staff drives increased use of locum staff, agency cover, and short-term contracts. While this provides short-term relief, it introduces higher costs and variable consistency. The NHS Long Term Workforce Plan notes that temporary staffing can negatively affect both patient experience and continuity of care.
Reduced productivity across the team
Turnover does not just affect the vacant role. Onboarding new staff takes time, supervision requirements increase, and experienced colleagues are pulled away from clinical work. This hidden productivity loss is rarely measured but widely felt across the team.
Leadership time spent firefighting

Constant recruitment becomes a growing leadership concern when managers spend more time filling gaps than improving services. Workforce gaps demand constant attention, and long-term planning is deprioritised. Leaders are forced into reactive decision-making rather than service development.
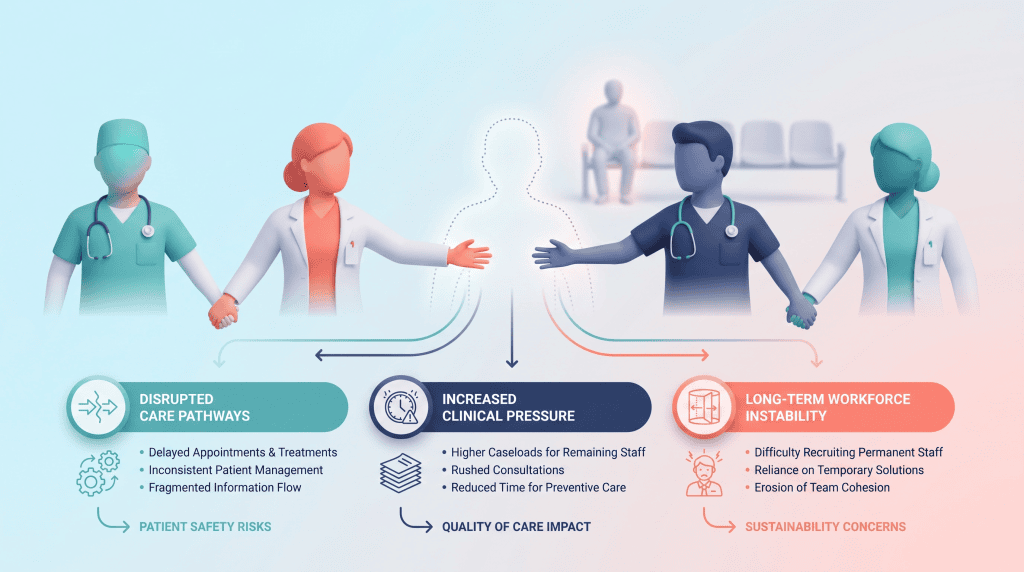
Disruption to workforce planning
Effective workforce planning depends on stability. When turnover is high, staffing models become unreliable, service delivery harder to predict, and financial planning less accurate. Even when roles are technically filled, frequent churn means teams rarely reach full effectiveness.
Why is staff retention in the NHS a growing priority?
Improving staff retention has become a key focus across the NHS. The King’s Fund NHS workforce data shows that while retention has improved recently, turnover remains a live operational issue. In primary care, this is especially pressing given increasing demand, limited workforce supply, and competition for skilled roles. Improving staff retention in the NHS is not just about reducing leaver rates – it is about building stable, supported teams that can deliver consistent care.
How can practices and PCNs improve staff retention?

Improving retention requires a proactive approach. Practices should provide clear role structures and expectations from day one, support professional development, and ensure the right skill mix across teams. Reducing unnecessary workload pressure and embedding structured recruitment and retention strategies are also key levers for improving stability.
High staff turnover doesn’t just create recruitment challenges. It affects continuity, productivity, and the ability of teams to deliver consistent care. For primary care organisations, stability is what allows services to run effectively and grow over time.
Adeem Azhar, Co-Founder and Chief Executive Officer – Core Prescribing Solutions
FAQs
Looking for support with your PCN pharmacy workforce?
If your PCN wants to build a stable, resilient team and reduce the operational impact of workforce churn, we can help. Our clinical pharmacist support integrates experienced Clinical Pharmacists and Pharmacy Technicians directly into your practice. We also offer opportunities to join a stable, specialist team for professionals seeking a supportive environment.


 01274 442076
01274 442076